Contents

You may think that since LH is essential for reproduction that it is no longer necessary once you pass that stage of your life. That is not the case, especially for men.
The Trusted sourceLuteinizing HormoneMerriam WebsterGo to sourceluteinizing hormone definition is as follows: a gonadotropin (sex organ affecting hormone) secreted by the anterior pituitary gland.
In this report, we will cover the following topics:
- Luteinizing hormone function in males and females
- How the body produces luteinizing hormone
- Impact of low and high levels of LH
- How to test luteinizing hormone levels and what is normal
- The best way to balance LH levels
Luteinizing hormone is a vital link in the process of reproduction.
What Is Luteinizing Hormone and What Does It Do?
Every hormone has a purpose in the body, and LH is no different. What is the function of luteinizing hormone, and how does it differ in men and women?
LH plays crucial roles in the reproductive cycle that are very different between males and females, as you will see below:
- Males
In males, luteinizing hormone directs the Leydig cells in the testes to produce testosterone. As a result, testosterone can then help with the process of spermatogenesis – the maturation of immature sperm cells vital for fertilization of an egg.
- Females
In females, luteinizing hormone regulates progesterone and estrogen production. During the first two weeks of the cycle, LH stimulates oestradiol production in the ovaries.
LH controls the length of the menstrual cycle. It is responsible for preparing the uterus for the implantation of the fertilized egg.
Another function of luteinizing hormone in females is to tell the ovaries that it is time to release a mature egg for fertilization. LH levels surge two weeks into the female menstrual cycle to Trusted sourceOvulation and conceptionThe Women`sGo to sourcecause ovulation . At this time, the ovarian follicle ruptures (tears) and the mature egg (oocyte) releases.
The remains of the ruptured ovarian follicle form the corpus luteum. If egg fertilization occurs, LH stimulates the corpus luteum to produce progesterone to support the early stages of the pregnancy.
Some LH receptors are also in the adrenal glands, which may help stimulate testosterone production later in life, especially in women after menopause.
Luteinizing hormone regulates the functions of the testes in males and the ovaries in females.
How Does the Body Produce Luteinizing Hormone?
The anterior pituitary gland produces luteinizing hormone in direct response to its receipt of luteinizing hormone-releasing hormone (LHRH) from the hypothalamus. The body has a unique system referred to as the hypothalamic-pituitary-gonadal axis. There is a negative feedback reaction that occurs when the hypothalamus measures blood hormone levels as follows:
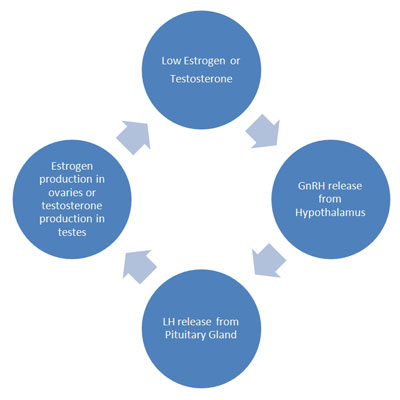
One difference that occurs in this cycle is that elevated estrogen levels during the midpoint of a woman’s cycle are higher, yet still stimulate an increased surge of luteinizing hormone levels to support ovulation.
Luteinizing hormone production is part of the hypothalamic-pituitary-gonadal axis that maintains crucial hormone balance in the body.
What Happens When Luteinizing Hormone Levels Are Low?
Any low hormone level can impact how the body functions. Decreased LH levels can result in the following issues:
- Male
Low luteinizing hormone in males can be indicative of a pituitary gland that is not making enough LH. That can result in reduced testosterone production and infertility. Low testosterone levels impair sperm cell maturation.
Younger males who do not produce enough LH during puberty might have slow sexual and bodily development as testosterone is essential for increasing muscle mass, growing body and facial hair, and enlarging the larynx to deepen the voice.
Kallmann’s syndrome in men is also indicative of low GnRH secretion from the hypothalamus resulting in decreased LH levels.
- Female
Luteinizing hormone levels vary considerably at different times of a woman’s menstrual cycle, which also affects its functions.
Low luteinizing hormone levels in women can prevent ovulation and cause menstrual period irregularity, and may also be due to any of the following:
- Anorexia or eating disorders
- Female athlete triad
- Malnutrition
- Pituitary disorder
- Stress
Low luteinizing hormone levels can lead to infertility in men and women.
Can You Have Too Much Luteinizing Hormone?
Just as hormone levels can be too low, they can also be too high. When that occurs, other issues may become problematic. What is luteinizing hormone going to do to the male and female body if the levels are too high? Elevated LH levels can indicate infertility in both men and women.
Below is a breakdown of what may happen in the body in cases of elevated LH levels:
- Male
Abnormally high levels of luteinizing hormone in men could indicate that the testicles are not using the hormone to produce testosterone, causing elevated LH to remain in the bloodstream.
- Female
Abnormally high luteinizing hormone levels at nonovulatory times of the menstrual cycle may indicate the onset of menopause. Other reasons for elevated LH levels in women include polycystic ovarian syndrome (PCOS) or pituitary disorder. Women with PCOS may have high testosterone levels.
Conditions such as Klinefelter syndrome and Turner syndrome can lead to elevated LH levels. These conditions may lead to infertility and an inability to reproduce. In Klinefelter syndrome (males), an extra X chromosome (XXY instead of XY) often causes smaller testes that do not secrete enough testosterone to support sperm production. Turner syndrome (females) is indicative of a partial or complete deletion of an X chromosome (XO instead of XX), resulting in impaired ovarian function. In these cases, the body often produces excess luteinizing hormone to stimulate testicular and ovarian functions.
Too much luteinizing hormone often indicates infertility.
How Do You Check Luteinizing Hormone Levels?
As with all other hormone levels, measurement is Trusted sourceLuteinizing Hormone (LH)Lab Tests OnlineGo to sourcethrough blood analysis . The luteinizing hormone blood test directly measures your LH levels to help the doctor determine why you are having symptoms of either low or high luteinizing hormone.
A test of your luteinizing hormone levels is called for if the doctor suspects any of the following to be an issue:
- Males – low sex drive or impotence
- Females – irregular periods, lactation when not nursing or pregnant
- Both genders – infertility, pituitary gland disorders
Your hormone doctor will measure many other blood hormone levels, including testosterone, estrogen, and follicle-stimulating hormone when checking LH levels.
Normal LH levels are as follows:
- Males – between 1.24 and 7.8 IU/L
- Females (during the follicular phase of the menstrual cycle) – between 1.68 and 15 IU/L
- Females (during midcycle peak) – between 21.9 and 56.6 IU/L
- Females (during the luteal phase) – between 0.61 and 16.3 IU/L
- Females (postmenopausal) – between 14.2 and 52.3 IU/L
Blood testing measures luteinizing hormone levels.
How Do You Balance Luteinizing Hormone Levels?
If your blood tests do not show a luteinizing hormone normal range, the doctor will then determine the appropriate form of treatment.
High LH levels in women are a sign of “primary ovarian failure,” meaning that the problem often originates in the ovaries.
Low luteinizing hormone levels in women are indicative of “secondary ovarian failure” where the hypothalamus or pituitary gland initiates the problem.
High LH levels in men are due to an issue with the testicles while low luteinizing hormone levels often deal with the hypothalamus or pituitary gland.
Elevated LH levels in women are often associated with PCOS, which can lead to insulin resistance. Managing insulin levels is one way a woman can help balance her LH levels. Exercise, consuming low glycemic foods, and using inositol and omega 3 as a supplement may help. Of course, proper guidance from a hormone specialist is crucial before using any supplements aimed at balancing hormone levels.
Caffeine affects luteinizing hormone levels that can be contradictory. While it increases LH output and decreases FSH secretion, it can also constrict the blood vessels. That can lead to reduced blood flow to the uterus that can impact pregnancy by preventing the fertilized egg from attaching to the uterine wall. Women trying to conceive may wish to avoid caffeine.
Testosterone therapy can also be used to help women make the ovarian follicles more sensitive to LH signals if luteinizing hormone levels are too low. Estrogen or testosterone replacement in menopausal women may help make up for low LH levels.
HCG and clomiphene are two treatments that can help stimulate natural testosterone production in men trying to conceive. In older men, testosterone replacement therapy can help increase testosterone levels.
Because hormone balance (testosterone and estrogen) is crucial as you age to protect your bones, brain functions, and more, the right treatment is essential.
- W. Paul Dmowski, MD, PhD, Parviz Rezai, F. J. Auletta, PhD, Annual Antonio Scommegna, MD
- Dr. Francisco I. Reyes, Jeremy S. D. Winter, Dr. Charles Faiman, MD
- Howard Jacobs, MD, FRCP, FRCOG, Dr. Corrina Wright
- Chad Haldeman-Englert MD, Maryann Foley RN BSN, Raymond Turley Jr PA-C
- Pratap Kumar and Sameer Farouk Sait
- Daniel Nedresky, Gurdeep Singh
Abnormal Follicle-Stimulating Hormone and Luteinizing Hormone Patterns Contrasting with Normal Estradiol and Progesterone Secretion in Women with Longstanding Unexplained Infertility
Pituitary-ovarian relationships preceding the menopause
Spontaneous pregnancy in a patient with hypergonadotropic ovarian failure
Luteinizing hormone and its dilemma in ovulation induction